
Up to 20 percent of people suffer at least once from hives, and the intense itching caused by the condition sends many sufferers to the emergency room in search of relief. Once they get there, they are often treated with a prescription antihistamine and the steroid prednisone. But a new study of emergency room patients, recently published online in the Annals of Emergency Medicine, asserts that adding prednisone is no better than an antihistamine alone in the treatment of hives.
The finding is important because prednisone is a powerful drug with a long list of severe and even potentially fatal side effects, including glaucoma, cataracts, high blood pressure, osteoporosis, suppressed adrenal gland hormone production and increased risk of infections, according to Mayoclinic.org. The most severe side effects occur with long-term use.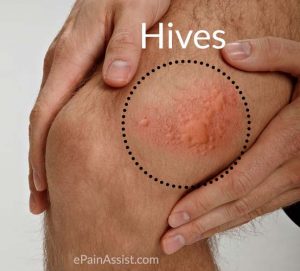
In the study, a follow-up assessment two days after treatment found 62 percent of patients treated with a combination of levocetirizine (a prescription antihistamine) and prednisone had an “itch score” of zero; however, 76 percent of those who received levocetirizine and a placebo achieved the same zero itch score.
Additionally, the study showed that the addition of prednisone to the treatment did not help prevent a recurrence of the hives, as 30 percent of patients in the prednisone group reported relapses, compared to 24 percent in the placebo group.
Dr. Patrick Ottuso, M.D., a Vero Beach dermatologist and fellow of the American Academy of Dermatology, is familiar with this study and others that have preceded it. He says there is some controversy in the medical community about the role of prednisone in the treatment of an acute case of hives – the type of attack that can precipitate a visit to the ER. Some studies indicate that prednisone can help boost the effect of antihistamines; even those studies express caution about the use of prednisone, due to its many side effects.
In a fact probably known to very few outside the healthcare profession, the medical name for hives is urticarial. Sufferers know well that hives are welts; pink swellings that can appear on any part of the skin, and even in the eyes or mouth. In an outbreak, an individual hive lasts a few hours, fades away without leaving a trace, and is replaced with new hives. While usually small, hives can join together to cover broad areas of skin. In addition to the often intense itch, hives can sometimes burn or sting.
Hives are very common; one in five people have at least one episode in their lifetime. A single attack of hives is often due to a virus or an infection; repeated attacks can be triggered by an allergic reaction to certain foods – including nuts, chocolate, fish, tomatoes, eggs, fresh berries or milk. Vero’s Dr. Ottuso says other causes of attacks are many and varied, including allergens (pollen, dander, insect stings), environmental factors (heat, cold, sunlight, exercise, emotional stress), and almost any type of medication.
Some people suffer from chronic urticarial (CU), which is when the hives persist for a long period of time or recur repeatedly over months or years. Although hives are considered chronic if they last more than six weeks at a stretch, studies have shown that many people with the condition have hives for months or even years on end.
CU affects about 1 percent of the population. Dr. Ottuso says the condition is exceedingly frustrating for both the sufferer and their dermatologist – in part because the vast majority of cases are “idiopathic,” meaning a cause cannot be determined. In many of these idiopathic cases, the best guess is that the sufferer’s immune system is overactive – it is attacking normal tissues of the body, resulting in hives.
While the cause of CU is mysterious, Dr. Ottuso says it’s still a good idea for a medical work-up to occur: a medical history should be taken, along with a physical exam that includes blood and urine tests and a skin biopsy. This can show if any underlying medical issue is present which may be contributing to the hives – such as thyroid or liver problems, sinusitis or skin conditions.
If no cause of CU can be determined, treatment has traditionally consisted of antihistamines and NSAIDs. In a newer approach, an injectable drug called Xolair is sometimes prescribed. Xolair is a “monoclonal antibody,” meaning that it is manufactured to mimic the natural antibodies found in the human body.
There is agreement in the medical community that prednisone has no place in treating CU. Dr. Ottuso says, “The many side effects of prednisone are well known, and commonly include nausea, vomiting, heartburn, trouble sleeping, and excessive sweating.” More serious side effects can also occur, including those listed above and others such as muscle pain, irregular heartbeat, swelling of the hands and feet, and even seizures. And people with diabetes have to be particularly careful, as prednisone can cause a spike in blood sugar.
Dr. Ottuso’s words of advice: “If you are having hive-like reactions that occur often, see a dermatologist or an allergist for a full evaluation. And if you are experiencing any swelling of the mouth, tongue or throat, get to an ER or call 911, as those reactions can interfere with your ability to breathe and could potentially be life-threatening.”
Dr. Ottuso’s practice is part of Vero Beach Dermatology, located at 1955 22nd Ave; the phone number is 772-299-0085.



